A significant association of DS with both death (HR 1.204 CI 1.019–1.423 p = 0.029) and discharge (HR 0.434 CI 0.414–0.456 p \(< 0.001\)) was noticed even when correcting for confounding factors (age, sex, chronic obstructive pulmonary disease, diabetes, PaO \(_\) ratio), is easy to collect and focuses on physiological quantities directly measured from the patient. Injury of pulmonary capillaries by thrombotic and inflammatory factors, obstruction of pulmonary blood flow in pulmonary circulation and lung areas with high V/. The final population consisted of 401 patients from seven ICUs. A competing risk Cox proportional hazard model was applied to test for the association of DS with two competing outcomes (death or discharge from the ICU) while adjusting for confounders. 
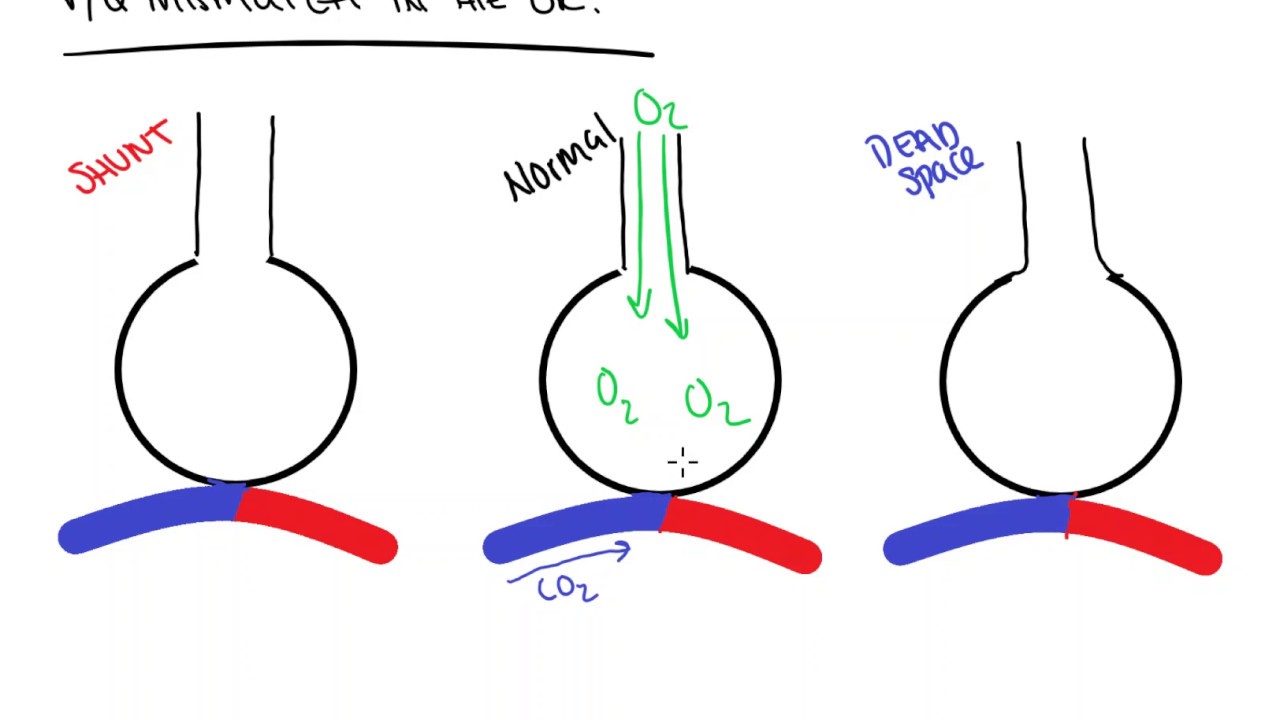
Basically dead space causes the hypercarbia because your effective minute ventilation is reduced from baseline. Retrospective cohort study on data derived from Italian ICUs during the first year of the COVID-19 epidemic. Dead space and shunt are just the extreme ends of the the V/Q equation. Here, we explore the association between a surrogate measure of dead space (DS) and early outcomes of mechanically ventilated patients admitted to Intensive Care Unit (ICU) because of COVID-19-associated ARDS. Physiologic dead space is a well-established independent predictor of death in patients with acute respiratory distress syndrome (ARDS).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
